Treatments for Myasthenia Gravis
Myasthenia Gravis (MG) is no longer considered a fatal disease. Most myasthenics, with the help of either drugs and/or surgery, lead near-normal lives.
However, there is no standard therapy for all myasthenics and there is still much to learn about MG – how it is diagnosed and how it is treated. As is usual with all things myasthenic, the success of one treatment over another is really dependant on the patient. What works for one person, may not work at all for another. And what works for one body part in a patient, may not work for another body part. A doctor may experiment with various therapies and prescription levels to achieve relief from myasthenic symptoms for the patient.
There is no one recipe for all situations, so the choice of treatment for an individual patient requires judgment and experience. Patients and their doctors are often required to make decisions even when the evidence is inconclusive. Patients need all the support which doctors, family and friends can offer.
Normally a neurologist is engaged for diagnosis and management of the disease. It would be helpful if the neurologist has extensive knowledge and experience in the management of MG (with the incidence of MG in only 1 person for at least every 10,000 people, it is highly likely that a number of neurologists have had little experience with this condition).
Current therapies for MG include:
- Anticholinesterase Therapy– an attempt to strengthen neuromuscular transmission with the use of drugs such as pyridostigmine bromide (Mestinon, Mestinon extended-release) and neostigmine (Prostigmin).
- Immunosuppressant Therapy – Prednisone; azathioprine (Imuran); cyclophosphamide (Cytoxan); cyclosporine (Sandimmune); mycophenolate mofetil (CellCept).
- Plasma Exchange – Plasmapheresis
- Intravenous Immune Globin
- Thymus & Thymectomy
- Other Therapies – atropine; pro-banthine; ephedrine
Hopefully, the neurologist will explain the various forms of treatment to the patient, and suggest the best way forward. There are advantages and disadvantages to each type of therapy, and the impact of the therapy could affect one’s ability to cope with the condition and such things as self image. Some factors to consider are:
- the patient’s current condition – for example, therapy for somebody in a myasthenic crisis such as breathing difficulties would be different to that for droopy eye lids.
- the patient’s reaction to the therapy – some medications may cause undesirable side effects such as nausea, dizziness and stomach pains and so could not be tolerated over long periods.
- the effect of the therapy on the patient’s ability to carry on with daily activities eg plasmapheresis requires hospital visits; thymectomy requires several weeks rest after surgery which could have an impact on income and ability to work.
- cosmetic implications – some therapies not only deal with the myasthenia, they will have other physical impacts – a thymectomy will leave the body scarred, some medications may cause bloating, or affect appetite.
Normally, the first treatment step is medication. There is no cure for MG, and so the drugs used to combat MG merely provide temporary assistance to help the body function normally. Additionally, the danger of using any drug is that the body may become tolerant of it over time, and so the drug becomes less effective. The choice is then to move to a stronger drug or to a different form of therapy, such as a thymectomy, which offers long term management of the condition.
In under 20% of myasthenics, MG goes into spontaneous remission which lasts longer than a year. No one knows why MG fluctuates or why natural remissions occur.
Anticholinesterase Therapy (Mestinon, Prostigmin, Mytelase)
Anticholinesterase drugs include:
- pyridostigmine (brand-name “Mestinon”)
- neostigmine (brand-name “Prostigmin”)
- ambenonium chloride (brand-name “Mytelase”)
We described the functioning of the muscle in the section What Causes Myasthenia Gravis. You might recall that for a muscle to contract, the nerve sends a message to the muscle through a neurotransmitter substance called acetylcholine (ACh). The nerve end releases a large amount of ACh, which travels through the neuromuscular junction (NMJ) (the gap between the nerve and the muscle) and binds to a receptor on the muscle membrane. In MG, the attacking antibodies bind to the muscle’s membrane and initiate a series of events that destroy the membrane and prevent ACh from binding. If ACh cannot bind to the muscle, the muscle does not receive the message from the nerve and will not contract.
Anticholinesterase drugs boost the body’s ACh by blocking the enzyme which usually breaks down ACh. This allows the build up of ACh to concentrate at the at the muscle receptor, which is where it is needed to transmit messages from the nerves to the muscles, and its effect is prolonged.
The most commonly used anticholinesterase is “Mestinon”. This comes in 60 milligram (mg) or 10 mg tablets and is released immediately. “Mestinon TimeSpan” is a 180 mg tablet in which 60 milligrams is released immediately and the remaining 120 milligrams are released over several hours. TimeSpan is usually prescribed for patients who require medication throughout the night (this allows for comfortable, uninterrupted sleep and reasonable strength in the morning). Timespan’s uneven release provides less predictable results than with ordinary Mestinon and is usually not recommended for day time use, but some myasthenics prefer taking it. Liquid “Mestinon” syrup is for children and for adults who have trouble swallowing pills.
There are no fixed dose or time schedules for anticholinesterases as muscle involvement and severity vary so much among myasthenics. An increase in muscle strength is usually noticeable within 20 to 40 minutes after taking the medication, and they produce their maximal effects about one to two hours after ingestion (although muscle strength rarely returns to normal). The effects start wearing off after three or four hours. The medication must be taken at regular intervals so that muscle strength is maintained throughout the day. For those myasthenics who have trouble chewing or swallowing, it is best to take medication at a time that will produce optimal strength during meals.
The need for anticholinesterases varies from day-to-day, and during the same day in response to infection, menstruation, emotional stress, and hot weather. Different muscles respond differently; with any dose, certain muscles get stronger, others do not change, and still others become weaker. A “brittle myasthenic” may be adequately medicated during one 3 to 4 hour period and over-dosed with the same dose in the next 3 to 4 hour period. Medication dosage may require frequent adjustment according to one’s response to the drug and to hourly/daily activity level.
Anticholinesterases are the gentlest of the drugs available to treat MG. However, some people do experience side effects, including:
- stomach cramps
- queasiness and nausea
- gut hyperactivity and diarrhea
- vomiting
- increased perspiration
- increased salivation
- muscle twitching and muscle cramps
- palpitations
- increased urinary frequency
- the muscle controlling the pupil of the eye is also affected, and there may be difficulty in focusing
- there are Acetylcholine receptors in the heart and so Mestinon may cause a very slow heart beat, which can, in turn, cause dizziness.
The presence of these symptoms may be a sign of taking too much medication, in which case the medication should be taken at longer intervals or in lesser amount. Other symptoms of overdose could include the worsening of generalized weakness, swallowing difficulties and respiratory failure (in which case a doctor should be contacted immediately). The myasthenic who is prescribed large daily dosage of anticholinesterase and suffering severe side effects or a worsening of their condition should question their doctor about their therapy.
To lessen the side effects, the drug can be taken with bland foods such as crackers and milk. If the unwanted side effects are particularly intense, they can be prevented or reduced by simultaneously taking other drugs – either anticholinergics (atropine) and hydrozyzine (Vistaril). It is also important to emphasise that all the unwanted effects of Pyridostigmine are short-lasting, and that it does not cause any permanent or long-term problems.
Immunosuppressant Therapy
As the name suggests, immunosuppressant drug therapy attempts to suppress the body’s immune system, although no one really knows how they work in MG. They are commonly called steroids (those used for MG are properly known as corticosteriods, not the anabolic steroids used by sports people). Steroids and other immunosuppressive drugs are often very effective in producing remission of symptoms.
The immune system produces antibodies to fights against foreign bacteria and viruses. In illnesses such as MG, the antibodies become overactive and start attacking the body’s tissues. Immunosuppressive drugs suppresses the production of antibodies to stabilize an overactive immune system. In MG, it is the ACh receptor antibodies that are suppressed, therefore allowing the receptors to regenerate and function in neuromuscular transmission. Hence, there is a return of muscle strength.
In the use of immunosuppressants, the best responses occur in patients with recent onset of symptoms, but patients with chronic disease may also respond. The severity of disease does not predict the ultimate improvement.
In decreasing order of their frequency of use in MG, they are:
- prednisone
- azathioprine (“Imuran”)
- cyclophosphamide (“Cytoxan”) and
- cyclosporine (“Sandimmune”).
Except for prednisone, none of these drugs is endorsed by its manufacturer specifically for treatment of MG.
Unfortunately these drugs can make it harder for the body to fight infection, and can also have serious effects, especially after prolonged use.
Prednisone
Prednisone is a synthetic drug which resembles natural hormones produced by the cortex of human adrenal glands, and is used to treat many illnesses. The body depends upon these hormones, called corticosteroids or “steroids,” during stress.
Unique to MG is the possibility of increasing weakness during the first two weeks of prednisone therapy, which requires close medical supervision when first administered. Some doctors try to avoid this initial weakening by starting with a low dose of prednisone and gradually working up to a recommended amount of 50 to 60 milligrams every day for several months. Onset of improvement in muscle strength usually occurs within 2 weeks but may take as long as 2 months. Marked improvement or complete relief of symptoms occurs in more than 75% of patients treated with prednisone.
When prednisone is taken in doses higher than 20 milligrams daily for longer than a week, the body’s natural production of adrenal hormones begins to decrease. This is called “adrenal suppression,” and is an undesirable but inevitable effect of taking high doses of a synthetic steroid. Once this occurs, prednisone cannot be stopped all at once but must be slowly tapered down over several months to give the adrenal glands a chance to “wake up” and begin producing natural adrenal hormones again.
Prednisone has a great many potential undesirable effects, usually related to dose and duration of drug use. In order to lessen the chance of undesirable effects, a gradual transition to alternate-day therapy is made after about two months of daily therapy, so that eventually twice the usual dose is given every other day for several more months. As soon as is feasible (3 to 12 months), the drug is very slowly tapered over many months to a long-term maintenance dosage (around 5 to 10 milligrams every other day) sufficient enough to keep myasthenic symptoms at bay. The choice of prednisone therapy is thus a long-term commitment lasting several years.
30% of myasthenics on high-dose prednisone therapy experience a drug-dependent symptom-free remission, and another 50% obtain marked improvement. However, 25% of patients also experience serious complications from this drug.
The side effects of using Prednisone (and any other steroid) are:
- Risk of developing osteoporosis – this is probably the most serious long-term effect. It results in thinning and consequently in weakening of bones and particularly those of the spine and the pelvis. The effect is worse in those who are already at risk of thinning of their bones such as the elderly or women past the age of childbearing. Exercise, particularly weight-bearing exercise such as walking and aerobics, is highly recommended (although some myasthenics may find this difficult). Diet should be high in calcium, protein and Vitamin D. There are now also available drugs (such as etidronate) which are being used successfully to treat bone thinning.
- Increased susceptibility to diabetes – steroids make the body less capable of dealing with glucose and other sugars, which affects diabetic patients. It may also induce mild diabetes in patients who didn’t previously have it. Strict dietary control may be necessary to counter this side effect.
- Thinning of skin and wasting of muscles – steroids tend to break down body tissues, and deplete them of protein. This can be counteracted by strenuous exercises, which again may be difficult for people with MG. Thinning of the skin leads to it being easily cut or broken, delayed healing of wounds, and also to increased susceptibility to the affects of sunlight.
- Increased risk in developing glaucoma and lens.
- Irritation of stomach lining and gullet causing indigestion, increased acid in the stomach and possibly ulcers.
- Sodium and water retention, causing some puffiness or swelling
- Other side effects include:
– mood changes and insomnia
– increased appetite and weight gain
– decreased resistance to infection
– high blood pressure
– increased sweating, especially at night
– increased hair growth
– acne on the face, back, and chest
– thrush (Candida) growth in the mouth
Patients on prednisone should:
- watch their weight
- keep as active as possible
- eat a balanced diet (high in protein, calcium and potassium but low in salt, free sugar and fat)
- stay out of crowds in enclosed areas (to avoid people with infections)
- see their doctors regularly.
Azathioprine (brand-name Imuran)
Imuran also suppresses the production of ACh receptor antibodies. It is used an alternative to prednisone where the patient either cannot tolerate prednisone or does not respond to it. Others respond better to treatment with both drugs than to either alone. In some patients, imuran is used as an aid to decreasing the dosage of prednisone.
The beneficial effects of Imuran seem to take months to occur, and often emerge so slowly and subtly that they are apparent only in retrospect. Because the response to Imuran is delayed, both prednisone and imuran may be started simultaneously with the intent of rapidly tapering prednisone when Imuran becomes effective. If Imuran is working, after about 3 to 12 months (or even longer in some patients), the myasthenic should notice a gradual improvement in how they feel. This improvement can be measured clinically by:
- Decrease in the number or severity of symptoms
- Need for less prednisone or Mestinon
- Need for less frequent plasmapheresis treatments
- Lower AChR antibody titer
Remissions which occur on Imuran are drug-dependent. Imuran is a long term treatment and a patient may have to stay on this medication indefinitely. Once improvement begins, it is maintained for as long as the drug is given, but MG symptoms recur 2 to 3 months after the drug is discontinued or the dose is reduced below therapeutic levels.
As with any immunosuppressive drug, it is important that the patient take Imuran exactly as prescribed by their doctor.
The undesirable effects of Imuran are less varied than those of prednisone but they can be very serious:
- Some people have a hypersensitivity or allergy to Imuran and develop fever, chills, joint and muscle pains, vomiting and dizziness. This usually occurs soon after commencement of treatment. When this unwanted reaction occurs, treatment must be stopped and cannot usually be restarted.
- Women who may want to have children should avoid this drug, because it has a known potential for producing fetal deformities.
- Imuran depresses the formation of new blood cells, just as it depresses antibody forming cells. It is therefore necessary to have complete blood counts of red and white cells frequently at the start of treatment, and three to four times a year once treatment is established. If the count drops significantly, it may be necessary to stop treatment temporarily.
- Liver function may be upset by Imuran. This can be monitored by blood tests. The effects are reversible on stopping treatment or reducing the dose.
- Susceptibility to infection – as Imuran depresses immunity, it increases susceptibility to infections. Special care must be taken to avoid contact with shingles and chicken pox which are much more severe in patients with lowered immunity.
- There is still much to learn about Imuran, including answers to such worrisome questions as whether it may increase the risk for cancer many years later. This is the most controversial, unwanted effect of Imuran. There are reports of an increased frequency of tumours mainly of the lymph glands in patients with rheumatoid arthritis taking Imuran. The sort of tumours that occurred in these patients were those that respond well to treatment once Imuran is stopped. However, a more recent report in 755 patients taking Imuran for bowel disease and who were followed for up to 29 years found no increase in the number of tumours of any sort. There are no comparable figures for MG Patients, but, on the basis of current knowledge, there is little cause for alarm.
Approximately one-third of patients have mild dose-dependent side effects that may require dose reductions but do not require stopping treatment.
Imuran is generally tolerated without serious adverse effects. The patient should check with the doctor immediately if any of the following occur:
- Nausea and vomiting
- Fever or chills
- Loss of appetite
- Upset stomach
- Skin rash
- Diarrhea
- Cough or shortness of breath
- Cold sores in the mouth or on the lips
- Blood in the urine or stool
- Unusual bruising
- Fatigue
- Missed menstrual period
- Yellowing of the eyes and skin
- Hair loss
- Muscle or joint pain
- Darkening of the skin and fingernails
More information about Imuran can be found at: www.gsk.com.au/gskinternet/publishing.nsf/Content/Imuran
Cyclophosphamide (brand-name Cytoxan)
Cytoxan is considered only for the most severe cases of MG when other therapies have failed. It is used either intravenously and orally for the treatment of MG.
Whilst experience from the Philippines reports good results with complete drug-free remission for a year and a half in three out of four MG patients who were treated with Cytoxan, the side effects are common and can be quite serious. They include:
- hair loss (almost universal occurrence on the drug)
- risk of bladder hemorrhage and bladder cancer.
These effects may be reduced by having the drug taken intravenously or orally once a week instead of daily. This drug usually requires the assistance of a rheumatologist or oncologist who is more familiar with it than are most neurologists.
Cyclosporine (brand-name Sandimmune)
Sandimmue is an immunosuppresion used during organ transplantation, and could be of benefit to myasthenics in reducing the dose of prednisone. A preliminary study without prednisone suggested that such a dose of cyclosporine could produce significant improvement in some MG patients if they could tolerate the side effects of this medication, the most prominent of which are elevated blood pressure, headaches, and increased body hair.
Most patients with MG improve 1 to 2 months after starting cyclosporine and improvement is maintained as long as therapeutic doses are given. Maximum improvement is achieved 6 months or longer after starting treatment. After achieving the maximal response, the dose is gradually reduced to the minimum that maintains improvement.
Adverse effects of this medication include:
- renal toxicity
- hypertension
- many drugs interfere with Sandimmune metabolism and should be avoided or used with caution.
Mycophenolate Mofetil (CellCept)
CellCept is a relatively new immunosuppressive drug that was originally developed to prevent immune rejection of transplanted organs. Whilst its treatment of MG is still being investigated, it appears that it may be of assistance to myasthenics who have found prednisone and other immunosuppressive drugs ineffective.
In a pilot trial conducted by Dr Donald Sanders (director of the MDA clinic at Duke University in Durham, N.C.), 8 out of 12 patients on CellCept for several months gained strength or were able to reduce their need for prednisone. In another study, 92 patients in Chicago were prescribed the drug for 3 to 45 months. Improvement was seen in 67 of these patients, including 5 who went into complete remission.
The advantage of CellCept over other immunosuppressant drugs is reported to have more rapid onset and fewer side effects. The drug has been reported to cause birth defects in animals, and so women of child bearing age should avoid getting pregnant whilst on the drug as the effect on unborn babies is unknown).
Plasma Exchange (plasmapheresis)
Plasmapheresis is a blood purification procedure used to treat several autoimmune diseases. It involves the exchange of the blood plasma which contains antibodies and other substances that interfere with the transmission of nerve impulses and replacement with fresh or artificial plasma.
The need for plasma exchange, and its frequency of use is determined by the response in the individual patient. The procedure is expensive, time consuming and not totally risk free, and is not meant for long-term treatment. So why is it used?
- To stabilise the condition of patients in myasthenic crisis where the condition is life threatening.
- To reduce moderate to severe muscle weakness before thymectomy.
- Some myasthenics do not respond sufficiently to more traditional forms of treatments, and so plasmapheresis offers their only relief from near paralysis and life-threatening respiratory problems.
The course of the exchange normally involves six to ten exchange treatments over two to ten weeks. To access blood, one tube is inserted into a large vein (possibly in the crook of the arm), and another placed in the opposite arm or foot. Around 3 to 4 litres of blood (depending on one’s body weight) is removed from the first tube. The blood passes through a blood separator, which works in one of two ways – either by spinning the blood at high speed to separate the cells from the fluid; or by passing the blood through a membrane with pores so small that only the fluid part of the blood can pass through. The plasma, which contains the antibodies, is discarded. The red blood cells are returned in artificial plasma (albumin and saline solution) via the second tube. Anticoagulant is added to the blood to keep it from clotting, but most of the anti-clotting agent is removed prior to returning the blood to the patient. Treatment, which can be uncomfortable, but is not painful, can take 2 to 5 hours. The patient lies down only during treatment but is able to walk around before and after treatment.
Maximum improvement may be reached as early as after the first exchange or as late as the fourteenth, but exchanges do not have a cumulative benefit.
The following difficulties may arise during the procedure:
- Sometimes it is not possible to achieve adequate blood flow from veins in the arms. Therefore, alternative blood access, which might involve some minor surgery, will be necessary.
- Although the latest technology blood cell separators remove only a small portion of blood from the patient at any one time, the changes in blood volume or the type of replacement fluid utilized my make some patients feel dizzy or lightheaded. Patients should immediately tell the medical staff if they begin to feel uncomfortable or if they suffer numbness, tingling associated with the mouth, eyes, fingers or toes and leg cramps, dizziness and mental confusion (all of which may indicate a low blood calcium or potassium level). Tiredness usually occurs after treatment.
- The anticoagulant used to keep the blood from clotting and certain types of replacement fluids might cause a patient to notice a sour taste in the mouth, tingling around the lips, or sharp pains, like pins being stuck in the fingers or toes. Patients should immediately tell the medical staff if they have any of these symptoms.
- The procedure isn’t selective about which antibodies it removes, and so it may result in excessive suppression of the immune system. The body can replenish anti bodies in time, but day patients may have to take special precautions against infection.
- Patients with clotting disorders may not be suitable for this sort of procedure.
Plasmapheresis does not cure MG – it only temporarily reduces the level of circuiting antibodies that attack the neuromuscular junction. It does not prevent the production of more antibodies, and usually the patient is given medication to help combat the condition.
Intravenous Immune Globin
Intravenous immune globin (IVIG) is the opposite of plasmapheresis – instead of drawing off the offending antibodies, IVIG swamps the body with pooled gamma globulin antibodies from many donors.
The process does not require special equipment, and the usual dose is small (eg 400 mg per kilogram per day infused for five successive days). Whilst the mechanism of action remains unknown, IVIG is thought to have a nonspecific suppressive effect upon the production of antibody by the immune system. It produces rapid improvement to help patient through a difficult period of myasthenic weakness. In patients who respond, improvement begins within four or five days, and may be sustained for weeks to months.
The process is quite expensive, and like plasmapheresis, the treatment is short term. As with plasmapheresis, its use is really limited to critical patients or those who are not responding to traditional treatments. It should be noted that there is a theoretical risk of transmission of blood born infections, although this has not happened now for some years.
Adverse reaction occur in fewer than 10 percent of patients. Symptoms include headache, fluid overload, and in rare cases, renal failure. Plenty of fluids should accompany the treatments to minimize the severe headache which can occur.
The Myasthenia Alliance Australia (MAA) worked in collaboration with AusPIPS, to develop a patient-centred brochure explaining the uses of immunoglobulin
All organisations involved (AusPIPS, MAA, IDFA, IDFNZ, and Myeloma Australia) support and advocate for immunodeficient patients receiving this important therapy. Supported by an unrestricted educational grant from CSL Behring (Australia) Pty Ltd.
It is accepted that there is a connection between the thymus and Myasthenia Gravis (MG) but the reason for the connection is not fully understood.
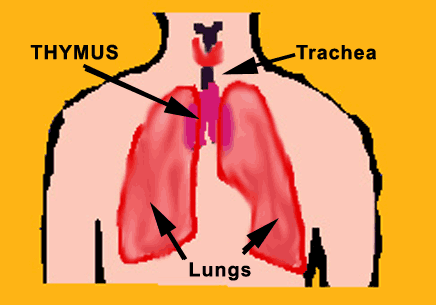
The thymus gland is an organ involved in the development of the immune system. It is located in the upper chest under the breastbone and is composed of many small lobes. During the formation of the fetus, the thymus migrates from the neck into the chest, and in adults it lies beneath the breastbone (sternum). Like tonsils and adenoids, the thymus is large in infants and gets smaller, to be replaced by fat, as we get older, making it hardly functional.
The myasthenic adult has thymic abnormalities. The thymus could be enlarged (as seen by CT scan) or it can contain more cells than normal (as seen under the microscope) – this is called hyperplasia and is often seen in myasthenics of many years standing.
Around 10% to 15% of myasthenics have tumours, called thymomas, which are usually relatively benign, but may become malignant. Thymomas are normally removed as soon as possible to prevent local spread (although, only around 30 to 50% of people with thymomas also have MG – and in some, MG develops after they have their thymectomy!). The risk of development of thymoma has led to thymectomy as well for MG patients without thymoma. (For more information on THYMOMAS, go to the Myasthenia Gravis Association UK website. There are two excellent papers by Dr Nick Willcox of the Institute of Molecular Medicine , University of Oxford on The Mysteries of Thymoma and MG.)
If most of the thymus gland is removed at surgery, myasthenic symptoms usually lessen and in some individuals go away completely. Although the relation of the thymus glad to myasthenia gravis is not totally understood, it appears that the thymus gland is linked to the production of acetylcholine receptor antibodies or other substances that interfere with neuromuscular transmission.
A thymectomy is the removal of the thymus gland by surgery. The goal of thymectomy as a treatment for MG is to induce remission, or at least improvement, permitting a reduction in immunosuppressive medication. Remission is the complete elimination of symptoms without medication.
Drug therapy, plasmapheresis and IVIG are short term treatments and do not completely relieve the symptoms of MG. They are beneficial, but in some patients may not be sufficient to allow the patient to return to full activity. Eventually the myasthenic with more than just mild disease, must decide on what to do next to attempt long term remission. This is especially true for patients with serious trouble swallowing or breathing, for whom long-term treatments may protect against rapid deterioration of these functions.
Most neurologists will therefore advocate thymectomy as the next step for the management of the condition – particularly for patients with generalised MG. Factors influencing the decision may include:
- age
- duration of the disease
- severity of the disease
- response to medication
- allergies
- cosmetic considerations.
In 1937, Dr. Alfred Blalock removed the thymus of a myasthenic patient when the thymus was found to have a tumour. He discovered that the symptoms of MG in the patient showed improvement. Since that time, thymectomy has been used as a normal course of treatment for myasthenics around the world, although the precise reason why it is beneficial is still not known.
In the past, it was thought that thymectomy would not benefit older patients (over 45 years old), or people who have had the disease for over 5 years. Yet some older patients and some long-standing MG patients have benefited from thymectomy, so now the recommendation for this procedure has to be considered on an individual basis. Although, there is uncertainty about the persistence of thymic tissue in such patients after the age of 60.
After a thymectomy, remission or marked improvement occurs in more than half of cases. Those who had thymomas do not usually improve as much as in young myasthenics without a thymoma.
Access to the thymus can be gained either by:
- transsternal thymectomy – the incision is made length-wise on the chest and the breastbone (sternum) is split open; or
- transcervical thymectomy where access is gained through the neck.
There are advantages and disadvantages to each approach. The splitting of the sternum is more traumatic than surgery through the neck, and the recovery time is longer, but it is more common because it more thorough allowing easier identification and removal of all thymic tissue (some doctors believe that leaving any remnant of thymic tissue in the body will increase the likelihood of the procedure failing).
About 30% of MG patients without a thymoma who undergo thymectomy eventually go into complete drug-free remission, and another 50% experience marked improvement. This improvement usually does not occur immediately after surgery, but may take up to several months or years to reach its peak effect. You cannot predict beforehand who will benefit from thymectomy, and even after benefit occurs there is still a small possibility of subsequent relapse. However, thymectomy itself rarely worsens the long-term course of MG.
Even invasive thymomas are not always detected with imaging tests and have been discovered during thymectomy surgery. Such experiences would argue in favor of eventual thymectomy over immunosuppressive drug therapy in otherwise healthy young or middle-aged MG patients, once the patient is up to the surgery. The possibility of an eventually complete symptom-free remission after thymectomy without the need to take any drugs, compared to a remission dependent upon the continued treatment with immunosuppressive drugs, is another significant advantage of thymectomy.
It is normally preferred that children wait until puberty before undertaking thymectomy because of the established role of the thymus in development of the immune system.
The process for a thymectomy is as follows:
- An x-ray is taken of the patient’s chest to determine the location of the thymus and to determine the existence of a thymoma.
- An anesthetist will consult the patient about the anesthesia plan – how the patient will be put to sleep, the use of any special drugs that will be needed to help the patient relax before surgery, and how the patient will generally feel after surgery. It is important that the patient tell the anesthetist about any allergies or reactions to any foods or medicines.
- Food and fluids will be withheld after midnight, or on the day of surgery. Routine medication for Myasthenia may or may not be given.
- On the morning of surgery, a pre-operative medicine may be given by injection. This medication can cause relaxation, drowsiness, and dryness of the mouth.
- After surgery, a one to three hour stay in the recovery room is required. The patient will then be transferred to Intensive Care Unit for 12 to 24 hours to ensure that everything is proceeding normally. In this phase of the recovery, fluids and medication will be given by means of a needle in the vein called an intravenous, or I.V. They will then be transferred back to their ward. Very occasionally if the patient has some breathing difficulties he or she may temporarily be connected to a ventilator so as to ease this problem.
- Once fluids are tolerated by the mouth, the intravenous fluids will be stopped. Solid foods will be started slowly, and the patient’s medication will once more be given by mouth. If progress is maintained, the patient will probably be allowed home in 7 days (although length of stay in the hospital varies for each patient).
- Most patients complain of some chest soreness and pain after surgery. This can be lessened with pain medication. At intervals, the patient will be asked to do coughing and deep breathing exercises to clear the lungs of mucus. This does cause discomfort which can be lessened by hugging a pillow and supporting the chest while coughing. Pain medication can be taken prior to any activity or exercise to alleviate after-surgery discomfort.
- The recovery period away from work varies. Most patients take 4 – 6 weeks off work for convalescence. Those with jobs which require heavy lifting or any strain on the chest may need a longer recovery time so that the chest is more fully healed before starting work. The patient should discuss this with the surgeon prior to the surgery in order to plan the recovery time.
After surgery there may be an increase in muscle weakness in some patients. However, treatment will be adjusted to meet individual needs.
Thymectomy may lessen the severity of the myasthenic symptoms; however, the degree to which the symptoms are lessened differs in each patient. The mechanism by which thymectomy produces benefits in MG is still uncertain. In general, ACh antibody levels fall after thymectomy, although there are conflicting reports. A study published in 1983 study findings found as high as 85% of patients who underwent thymectomy showed clinical improvement, and the maximal favorable response generally occurs 2 to 5 years after surgery (but some people may experience better health 7 to 10 years after surgery). The best responses to thymectomy are in young people early in the course of their disease, but improvement can occur even after 30 years of symptoms. Patients with thymomas do not respond as well to thymectomy as do patients without thymoma. The worst response rate to the surgery was from those who had surgery when they were over 60 years of age.
When considering surgery, it is important for the myasthenic to tell their neurologist and their surgeon of any concerns – the length of time of surgery, the effects of the anesthetic, the resultant scar, after surgery care, pain management.