Diagnosis – how is Myasthenia Gravis confirmed?
The symptoms of Myasthenia Gravis (MG) are common complaints that can be found in a variety of medical and even psychological conditions. The symptoms include drooping eyelids, double vision, difficulty chewing or swallowing, weakness in almost in any part of the body, and even simple fatigue. One can see that the symptoms of MG are not specific to the condition. This can make it difficult to diagnose MG, particularly in cases where the condition is mild, or where the doctor is not familiar enough with MG to suspect the condition. Generally an individual with potential symptoms of MG would be referred to a neurologist for diagnosis, but sometimes an ophthalmologist or an immunologist will also make the diagnosis.
There are many different kinds of disorders that can cause symptoms similar to MG, and so a complete history and both general and neurological examination are important first steps in diagnosing MG and ruling out other disorders. This may include a careful family history, past medical history and medication history; as the disorders that can mimic MG can occur for many different reasons. It may therefore be important that your doctor has access to your previous medical records and any previous tests, in particular this includes scans and x-rays. This section does not address the tests that might be required to investigate potential diagnoses other than MG.
It is not often realised that there is no single test that absolutely proves the diagnosis of MG. However, the combination of history, clinical examination, nerve tests and blood tests often establishes the diagnosis beyond reasonable doubt. If there is doubt after the tests have been completed often a trial of treatment for MG helps clarify the issue, and the diagnosis also often becomes clearer in the longer term.
Clinical History
The doctor should know as much as possible about all symptoms that the patient is experiencing. The patient should be quite specific about what symptoms are occurring, the time of day, the circumstances, what brings it on or makes it better, and what is actually felt. If specific muscles are more affected let the doctor know. If the doctor suspects MG, further tests are usually carried out.
There are certain symptoms that are more suggestive of MG. These include:
- double vision or drooping of the eyelids that comes and goes, particularly if it is worse towards the end of the day
- speech becoming weak or nasal after a few minutes of use
- difficulty with chewing or swallowing that gets worse after a few minutes or with something difficult to chew, such as steak
- the head suddenly dropping forwards without the patient feeling sleepy
- weakness in the shoulders or hips that gets worse towards the end of the day
Neurological Exam
A neurological exam can involve many things, but if MG is suspected it will be focused on the findings that may occur in MG.. The doctor may also look for the findings that may indicate an alternative diagnosis. An examination focused on MG will test various general areas: the eyes, speech and swallowing, the neck, and the arms and legs, plus other things as determined by the circumstances. The concept of fatigability is particularly important for MG, and this is when the muscle is initially strong but after some seconds becomes weaker.
- In the eyes the doctor might check the eyelids for drooping, the eye movements for limitation or double vision, the strength around the eyes and of facial movements, plus the ability to look up for a sustained period of time to test for fatigability of the eye and eyelid movements.
- In the throat the doctor might check for the tone of the voice, the ability to talk for a sustained period, the ability to hold a sung note, and the ability to safely swallow and drink. The doctor might also examine the thyroid gland at the front of the neck, and the strength of the neck in pushing the head forward and back against resistance.
- In the arms and the legs the doctor might check for the presence and symmetry of reflexes, strength in the muscles particularly in those around the shoulder and hip, the ability to do certain things such as rising from a chair without using arms to help, and the presence of fatigability by checking strength in one side for a sustained period and then comparing it after that to the other side.
Clinical Tests
There are two special clinical tests that the doctor might perform looking for MG. These are the ice test and the Tensilon test. In the ice test the doctor will examine for improvement in eyelid drooping after covering the eye for a minute or two with an ice pack or a cold pack. In the Tensilon test the doctor will examine for improvement in any weak area of the body after administration of the medication Tensilon. This medication only works when injected into the vein, and only has a short duration of effect. Variations on this test include the injection of neostigmine, and taking a tablet of Mestinon, again see if there is any improvement of weakness. Obviously both the ice test and the Tensilon test require something abnormal to be present at the time of the test, in other words the tests cannot be done if there are no abnormal findings on examination at the time.
Nerve Conduction Studies and Repetitive Stimulation
Nerve conduction studies can test both the sensory and the motor nerves, in the context of MG generally only the motor nerves are examined. An electrical stimulus (shock) is applied to the skin overlying the nerve, the nerve then activates and sends the signal to the muscle supplied by that nerve. The size of the muscle response and the time that the nerve signal takes to get there is recorded from a separate set of electrodes on the skin over the muscle.
This test often frightens people but it sounds worse than it actually is, and the doctor will generally have established normal ranges on themselves and will know what it feels like.
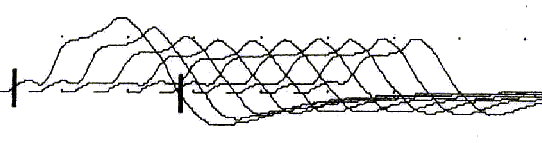
In MG repetitive closely timed stimuli will often produce progressively smaller or weaker responses in the muscle recording electrodes. This is called Decrement of the Compound Muscle Action Potential (CMAP) in the Repetitive Stimulation Test. It is the most specific of the nerve tests for MG, but is not present in all cases and is only able to be done on certain muscles, which may not be affected in any individual patient. An example of decrement on repetitive stimulation can be seen below, with progressive decline in size (and therefore power) in the first four muscle responses. This is the electrical, objective equivalent of the fatigue that most patients with MG experience.
In some instances an electromyogram (EMG) will also be performed, particularly if an alternative diagnosis is being considered. An EMG involves placing a very tiny electrode needle into the muscles, and the muscle will then be examined both with the patient relaxing the muscle and with the patient activating the muscle. Always let your doctor know if you are on blood thinning agents, in particular warfarin, before having this test as a more limited EMG test may be done in such circumstances.
For more detail on EMG results, see http://www.neuro.wustl.edu/neuromuscular/mtime/mgdx.html#rns)
Single Fibre EMG (SFEMG)
SFEMG is the most sensitive nerve test of neuromuscular transmission and shows increased jitter in some muscles in almost all patients with myasthenia gravis. SFEMG is like standard EMG in that a small needle is inserted into the muscle. However it is technically a much more difficult test for the doctor and often requires a study of up to an hour long. For this reason generally the other tests are done first, and SFEMG is used if the other tests are normal but the diagnosis of MG is still suspected.
The concept of jitter and exactly what causes it can be difficult to explain without a thorough knowledge of the nature of the neuromuscular junction. Muscles are made up of thousands of separate muscle (motor) units. Jitter can be thought of as a measure of the fatigability within a microscopic single motor unit itself, rather than within the muscle as a whole which is tested with repetitive stimulation. The tiny needle is actually inserted within a single motor unit.
Jitter is greatest in weak muscles but may be abnormal even in muscles with normal strength. Patients with mild or purely ocular muscle weakness may have increased jitter only in facial muscles. Increased jitter is a nonspecific sign of abnormal neuromuscular transmission and can be seen in other motor unit diseases. Therefore the finding of increased jitter does not definitely mean that MG is present. Normal jitter in a weak muscle excludes abnormal neuromuscular transmission as the cause of weakness.
Blood Test for Serum Antibodies to AChR
Blood tests can be performed to help in the diagnosis of MG. This is not a routine blood test that a general practitioner would necessarily do, and is not ordered as part of a routine blood screen or during a routine medical. It can however be done on a standard blood sample, although it is only done in a few laboratories in Australia.
The standard MG blood test is the detection of serum antibodies to the acetylcholine receptor (AChR antibodies). Antibodies are proteins made by the immune system that are able to bind specifically to other proteins. In the case of MG, the antibodies bind to the acetylcholine receptor protein and block its function or damage it. As the acetylcholine receptor protein is a normal protein in the human body, the antibodies are often called autoantibodies and MG is called an autoimmune disease.
AChR antibodies are only detectable in about 50% of patients with MG confined to the eyes, and about 80% of patients with generalised MG, where it affects not only the eyes but also other parts of the body. This means that some patients with MG are missed by this blood test, and therefore it cannot be relied upon to detect all cases of MG. Technically this means the ACHR test has impaired sensitivity for the diagnosis of MG.
It should be noted that the concentration of AChR antibodies varies widely among myasthenics, and that the level of concentration does not predict the severity of the condition. Further, the level of AChR antibodies may increase as the condition progresses. AChR antibodies might very occasionally be elevated in people with systemic lupus erythematosus, inflammatory neuropathy, rheumatoid arthritis taking D-penicillamine, thymoma without myasthenia gravis, mothers of children with arthrogryposis congenita, and in relatives of patients with myasthenia gravis. However often when these patients are carefully examined clinically and with nerve tests they are found to have subtle MG without having realised it. Technically this means the ACHR test has relatively good but not perfect specificity.
The simple way to look at the ACHR antibody test is that an elevated concentration of AChR antibodies confirms a clinical diagnosis of MG, but a normal or negative result does not exclude the diagnosis.
Around 20% of all myasthenics with generalised features have no AChR antibodies detectable in their blood (“seronegative” MG). About half of these patients have recently been shown to have antibodies to another protein present at the neuromuscular junction, called MuSK (muscle specific tyrosine kinase). The role of the MuSK protein is still been clarified, but it seems to be important in forming and maintaining the structure of the neuromuscular junction. Antibodies to MuSK for patients in Australasia and Southeast Asia can be tested at the Molecular Medicine Laboratory, Concord Hospital, Sydney.
Comparison of Diagnostic Techniques
There is no one definitive test for MG. The doctor will do the tests that are necessary for the exact clinical situation, but each test has certain advantages and disadvantages that are indicated below:
- Sometimes the diagnosis is obvious on the history and clinical examination, although the doctor will generally also want to tests to help guide treatment and provide for the monitoring of the response to treatment
- the icepack test is simple and quick but only generally useful when there is eyelid drooping
- The Tensilon test is useful when only ocular and oral symptoms are present, but is not completely reliable and can generally only be done in hospital.
- Detectable antibodies to ACHR or MuSK are highly diagnostic of MG at the absence of such antibodies to is not exclude MG
- Decrement on repetitive nerve stimulation generally confirms MG but is frequently normal in patients with mild or purely ocular disease.
- The finding of increased jitter by SFEMG is the most sensitive clinical test for abnormal neuromuscular transmission and is abnormal in almost all patients with myasthenia gravis, but it does not prove myasthenia gravis and is present in a number of other conditions that affect the nerve and muscle and that can cause symptoms similar to that of MG.
Sometimes all of these confirmatory tests are negative in someone whose clinical examination seems to point to MG. In these cases, the doctor would diagnose “possible MG” or “probable MG”. In this case a patient would be monitored to see if the condition manifests itself and a diagnostic trial of treatment may sometimes be given.